November 2020 Updates
November 4thOctober 2020 Updates
October 16thOctober 7th
Click For 2019 Updates
Click For 2018 Updates
December Updates
December 21thNovember Updates
November 26thNovember 9th
November 8th
November 7th
October Updates
October 26thOctober 6th
September Updates
September 27thSeptember 19th
Click For 2017 Updates
September Updates
September 29thJuly Updates
July 24thJuly 1st
April Updates
April 24thMarch Updates
March 9thFebruary Updates
February 16thFebruary 2nd
January Updates
January 25thJanuary 19th
Click For 2016 Updates
December Updates
December 22ndDecember 11th
November Updates
November 1stOctober Updates
October 19thOctober 13th
September Updates
September 27thSeptember 23rd
September 18th
August Updates
August 24thAugust 22nd
August 6th
July Updates
July 13thJuly 10th
July 6th
June Updates
June 30thJune 24th
June 18th
June 11th
June 4th
May Updates
May 27thMay 18th
May 8th
April Updates
April 22ndApril 16th
April 8th
April 4th
March Updates
March 27thMarch 20th
March 13th
March 7th
Latest Update From Camilla
I’m finally home from the hospital! I know I’ve said that before and then had to turn around and go right back in, but this time I’m determined to make it stick.
Just to recap, I was inpatient for three weeks total. The first two weeks were to start the immunosuppressant drug for the colitis caused by my cancer treatments. The immunosuppressant took longer than expected to start working. (I am a procrastinator in all senses of the word, I guess.) Luckily, we did start to see results, and they sent me home on a Friday night about 10 days ago.
Word of advice: if you’re going to be discharged from a hospital, don’t go home on a Friday night. It is so much harder to get in touch with your doctors or get new prescriptions over the weekend. Poor Michael (that’s what we call him now; so many people said it so often that it just became part of his name) … Poor Michael was on the phone all weekend trying to get all the supplies and new prescriptions I needed.
While I was home that weekend, I was having a lot of side effects from the immunosuppressant. Not surprising. It does suppress your immune system after all. The worst was that the drug was burning my esophagus, and it was so painful that I couldn’t eat or drink by mouth. I have a high tolerance for pain, but this was capital-P Painful. I got very dehydrated. Monday, Michael took me to the doctor, and he admitted me again.
Since we did not expect me to be admitted again, we had not warned Mara, and I had not gotten to say a proper goodbye before leaving her with my parents. So, I spent the next hour crying and pouting and sulking and acting like a real baby. Michael let me vent. Parents of toddlers know that sometimes you just have to watch as they cry and pound on the floor. Eventually, I calmed down and realized that I was only a few exam rooms down from where I first got my cancer diagnosis on February 25, 2016. That put things in perspective. (Incidentally, Mara handled the news about my admission fine.)
We did not know how long I’d be in the hospital the second time (the estimate was “a night or two” - I was there a full week), and we had not prepared for another hospital stay, so Michael had to run home and pack a bag for me. Michael and I have never been one of those couples who packs for each other before vacations, but he did a surprisingly good job. Sure, he brought 6 t-shirts and only 3 pairs of pajama pants. Fine, he forgot my slippers. Yes, all my toiletries were in weird spots and hard to find. That’s ok. The only real issue was that he forgot to bring me a hairbrush, so after a full week in the hospital without a hairbrush, believe me when I tell you that I looked like every Winona Ryder mugshot.
One tiny(?) hiccup during my hospital stay - I was seeing a doctor on my GI team nearly everyday, and last Tuesday he performed two endoscopy procedures on me. And then, the next day, he tested positive for COVID! Fantastic! So after all my family has done to protect me from COVID this entire year, I’m the only one who has actually gotten exposed. (Actually, Michael was briefly in the room with the doctor too, but only for a couple minutes.) Michael’s first thought when he heard I was exposed was, “What an f-ing mess! You’re immunocompromised, mute, and now I can’t be at the hospital with you.” My first thought was, “Damn! I could have gone to the beach this summer after all!” I mean, if I was going to get exposed anyway, I might as well have seen the ocean, right? Although I don’t discount the severity of COVID, I’m not that worried about this exposure. The doctor had an N95 mask on every time I saw him. I haven’t had any symptoms. His wife hasn’t even gotten it (although now that I think about it, that’s going to be hard to explain if I do get it from him). I’ve had two negative tests since my exposure and this Friday will be 10 days without symptoms. After that, I will get to hug my parents again!
The hospital stay should have been shorter, but the immunosuppressant kept causing other weird side effects. I started getting migraines and tremors. My hemoglobin plummeted. Stuff like that. Each one needed a workup and treatment. I got an iron infusion. I had MRIs of my head and spine (normal except for some degeneration from age. Um, what? I’m a millennial!).
I’m fairly convinced that making a person who has a migraine get an MRI is illegal under the terms of the Geneva Convention. If not, we should definitely start using it as torture at Guantanimo. If you haven’t had one, MRIs are insanely loud. They sound like someone made a mix-tape of just construction site noises and the screeching sound dial-up internet used to make. The first scan takes up to an hour. Then, they pump you full of contrast, which I imagine is sort of like tie dye for your insides, and they do the same scan again, except this time it only takes five minutes for some reason they never explain.
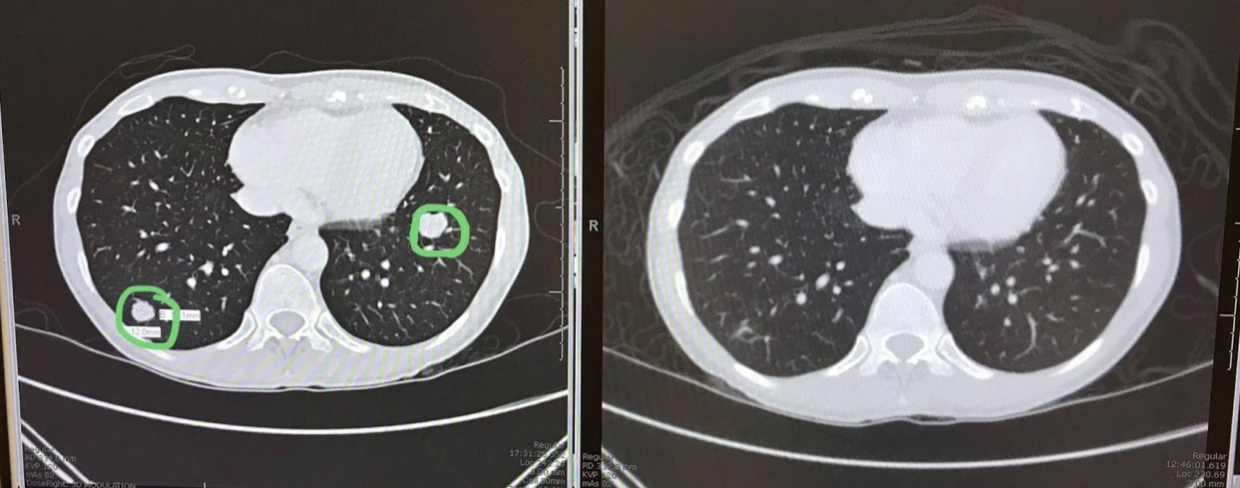
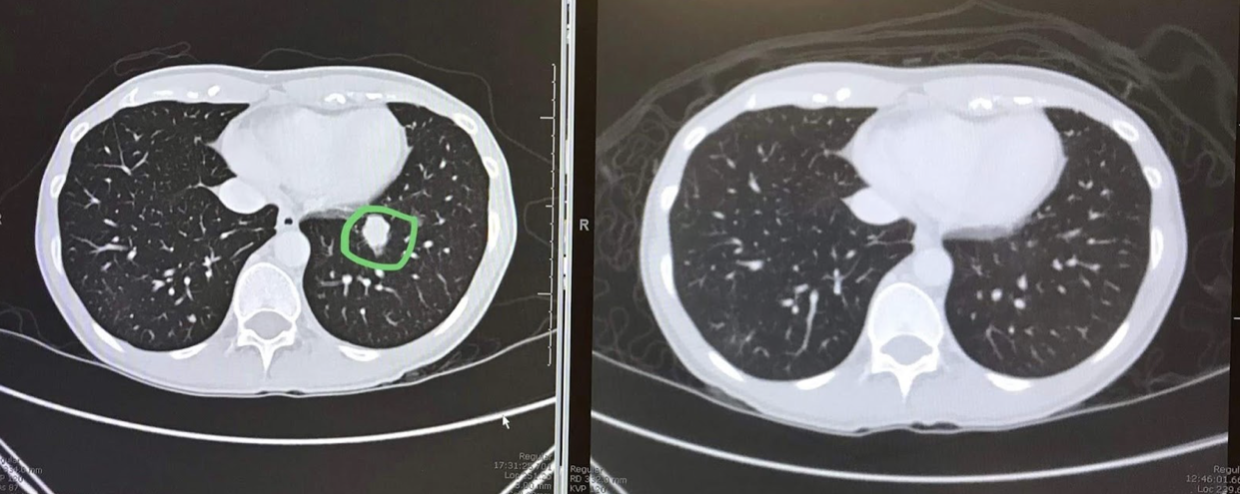
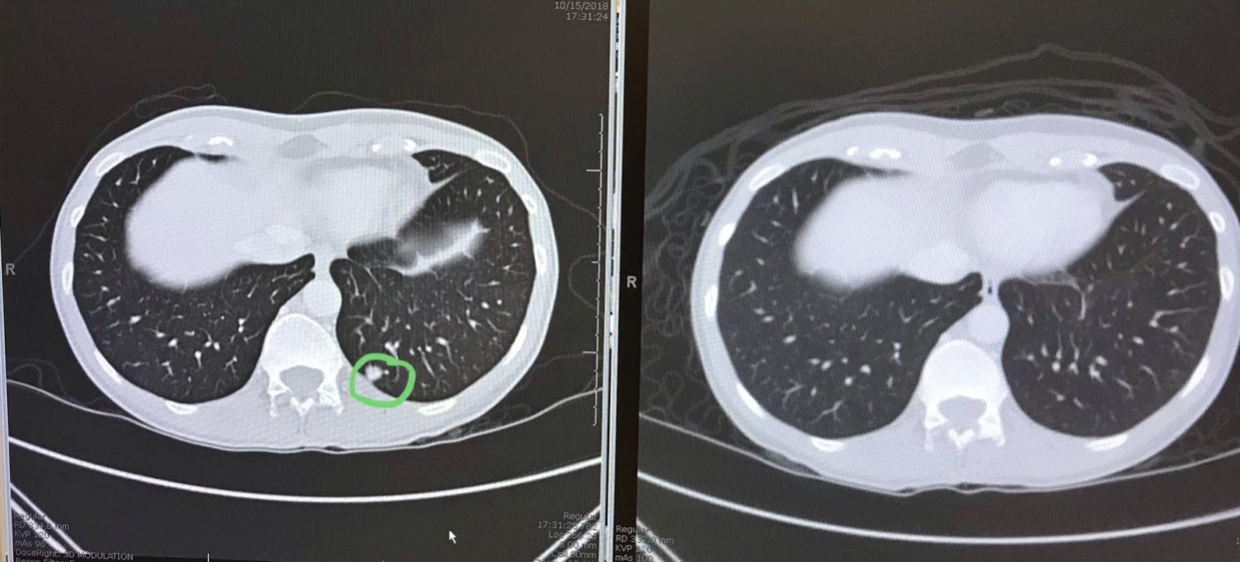
It takes about a hundred years to get the MRI report. When you get the MRI report, it will have a bunch of absolute jibberish sentences (“the enteoterioic hibiscus saline routes are parallel to the neurobiliac sac”) that you won’t be able to decipher even when you Google them, but, mixed in with those will be a bunch of basic statements like “Lungs are present.” These always catch me off guard. Like, was that a concern?
On Monday morning, I had been in the hospital a full week, and I was DONE. I hadn’t slept for more than two hours at a time. My body was covered in bruises from getting shots all week.
I texted my family: “I don’t care if the MRI shows a tiny alpine hiker rappelling down my spine. I am not staying in this hospital another night.”
Luckily, the MRI results were fine, and I was allowed to go home! I still have to be on tube feeds to get extra nutrition because it is still hard to swallow, and I still have a tremor. Michael keeps taking videos of it. He says they’re to show the neurologist, but I’m skeptical.
?It is wonderful being home with Mara and Michael. They have always been close, but I love watching the little rhythms they’ve developed while I’ve been gone. Mara’s desk is next to Michael’s desk, and she does her virtual learning next to him while he works. It is very cute. She doesn’t love the virtual learning, but she does love all the Facetime with our family. They’ve called to read, play, teach, and cook with her. It has been wonderful. She also loves all the food everyone has sent, and it has been such a relief to Michael to not have to worry about getting groceries or cooking. Thank you to everyone. I mean it when I say we could not do this without all of you.
One last thing I wanted to mention. I have had the most amazing nurses over the past four years. Out of the hundreds of nurses I’ve had assigned to me, there were only 3 that I didn’t think were great. I know there are a lot of people thanking Essential Workers and First Responders during COVID, but I just want to say that I witnessed first-hand how much extra work COVID is making for hospital staff - even with patients who don’t have the virus. Everyone, from maintenance to transport to nurses, has to take time to change gear constantly, put on extra gowns, take extra temperature readings, wipe down things more than usual. These are 12 hour jobs that were already chock full to begin with. If you know anyone in a hospital setting, even if they haven’t treated COVID patients directly, please thank them for all the time sacrifices they’ve been making to keep patients like me safe.
Oh, I lied. This is the last thing I want to mention. When I got cancer, a lot of people wrote to me to tell me about their cancer journeys. I never knew they were sick. When my cancer treatment caused colitis, a lot of friends messaged me to tell me they also have colitis or Crohn’s. I never knew they were sick. I am very open (probably too open) about my medical issues. Some of that is because I think it is good for people to know what is going on, and sometimes it is just easier because I can put all the information in one place and I don’t have to remember who I gave the details to. I get so much support and prayers from all of you because I’ve been so vocal (pun intended) about cancer. This time, I’d like to ask that you pray instead for someone who is sick but does not talk about it. They need the love and support. If you hear of a friend getting a diagnosis, even if they don’t complain or explain or joke or update like I do, they are still having a difficult time. If there’s anything you were thinking of offering me, please do it for them instead. That would make me so happy. You’re the best group of people, and I want to share you.